Ankle Sprain
Outcome: Re-injury
Comparison: Surgery (primary suture) vs Casting
Evidence snapshot
Volume
Data from 1,331 participants (9 RCTs)
Magnitude and Direction of effect
Statistical Fragility
Certainty of evidence
Support the project
If you found this evidence summary useful, you can support the continued development of independent evidence reviews.
Contributions help support ongoing literature surveillance, data synthesis, and site maintenance.
Evidence in detail
Inclusion criteria
- Randomized controlled trials
- Population: Adults with acute lateral ligament injury (high grade sprains / ligament tears)
- Intervention: Surgical repair (primary anatomical repair without augmentation)
- Comparator: Immobilisation (below-knee cast)
- Outcome: Re-injury (at least 6 month follow up)
Outcome definition and data extraction
Re-injury was defined according to the criteria used in each individual trial. Data were extracted at the longest reported follow-up. Analyses were conducted using the number randomised as the denominator, consistent with an intention-to-treat approach.
Effect measure and data pooling
Odds ratios were calculated for each trial and pooled using a fixed-effects model. Statistical heterogeneity was assessed using the I² statistic, which quantifies the proportion of variability due to between-study differences rather than sampling error. Statistical heterogeneity was low (I² = 28%, H² = 1.38), indicating that most variability in effect estimates was attributable to sampling error rather than true differences between studies.
Assessment of evidence quality and robustness
Risk of bias was evaluated using the PEDro scale. Statistical robustness was assessed using the Fragility Index, defined as the minimum number of event reversals required to alter statistical significance. Certainty of evidence was evaluated using the GRADE framework.
The analytical framework underpinning this Living Review, including statistical methods, fragility analysis, and certainty assessment, is described in the Methods page.
Results
Included trials
9 RCTs involving 1,331 participants were included. (Trial characteristics in Appendix 1)
Follow-up ranged from 6 months to 14 years.
Effect estimate
Surgical repair did not demonstrate a clear reduction in recurrent injury compared with immobilisation (OR 0.84, 95% CI 0.63 to 1.12; pooled data from 9 trials; p = 0.23). The confidence interval includes clinically important benefit in either direction, indicating substantial uncertainty regarding the comparative effectiveness of these strategies.
Forest plot
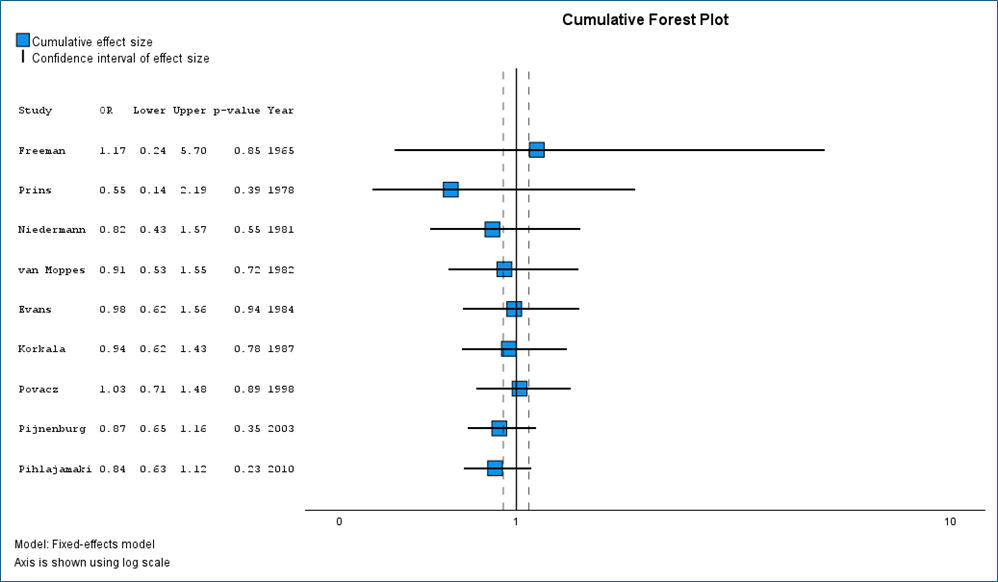
Fragility
Fragility analysis was not performed because the pooled estimate was not statistically significant; the Fragility Index is designed to assess the robustness of significant findings.
Publication bias
Trim-and-fill analysis did not identify any potentially missing studies, and no adjustment to the pooled estimate was required (Appendix 2). This suggests no statistical evidence of small-study effects; however, the power of funnel-based methods is limited when the number of included trials is modest.
Certainty of evidence
Certainty of evidence was rated as very low using the GRADE framework. Evidence was downgraded for very serious risk of bias, as most trials demonstrated methodological limitations (all included trials scored ≤5 on PEDro; Appendix 1), and for imprecision, as the pooled confidence interval spanned clinically important benefit in either direction. Consequently, the true effect may be substantially different from the pooled estimate. Further adequately powered, prospectively registered, methodologically robust trials are required to reduce uncertainty
Interpretation
The pooled analysis does not demonstrate a clear difference between surgical repair and immobilisation for preventing recurrent injury. The confidence interval spans clinically important benefit in either direction, indicating substantial uncertainty regarding the true comparative effect. Although point estimates suggest a possible modest benefit of surgery, the data are compatible with both benefit and no meaningful difference.
All included trials evaluated primary anatomical repair without augmentation, and the most recent study was published in 2010. Surgical management of lateral ligament injury has evolved, with increasing use of augmented repair and internal bracing techniques. These approaches were not represented in the included evidence base. The effectiveness of newer surgical techniques is examined separately [here].
Appendix 1: Characteristics of included studies
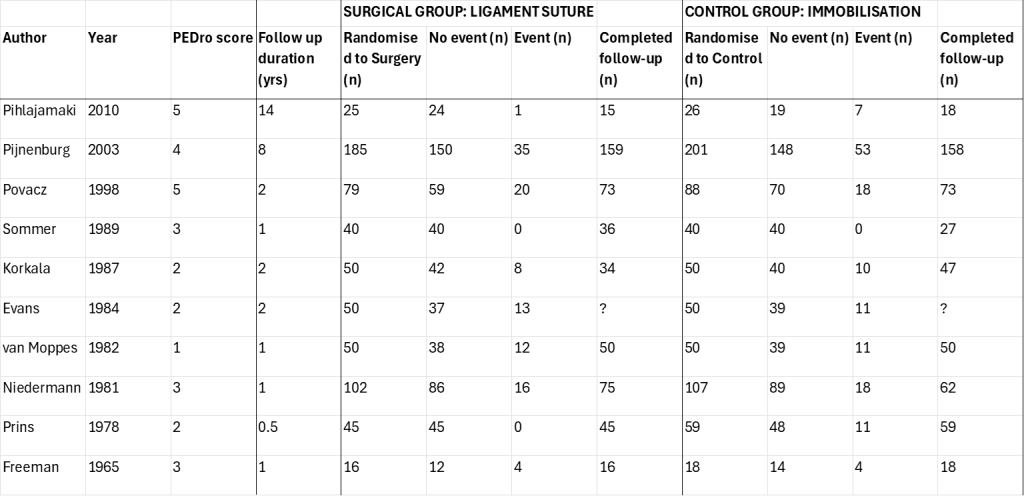

Appendix 2: Funnel Plot
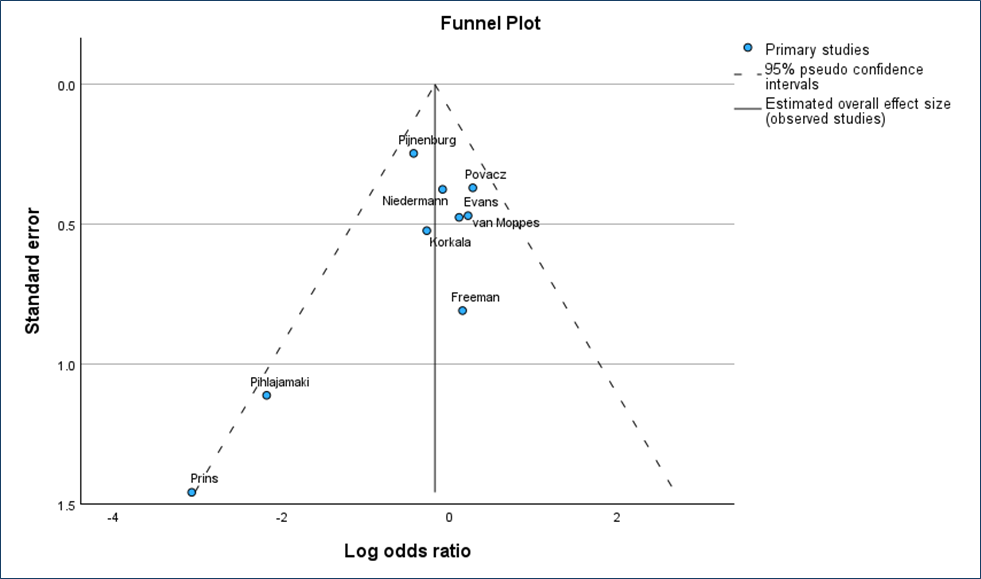
References (included studies)
Freeman MA. Treatment of ruptures of the lateral ligament of the ankle. J Bone Joint Surg Br. 1965 Nov;47(4):661-8.
Prins JG. Diagnosis and treatment of injury to the lateral ligament of the ankle. A comparative clinical study. Acta Chir Scand Suppl. 1978;486:3-149.
Niedermann B, Andersen A, Andersen SB, Funder V, Jørgensen JP, Lindholmer E, Vuust M. Rupture of the lateral ligaments of the ankle: operation or plaster cast? A propective study. Acta Orthop Scand. 1981 Oct;52(5):579-87. doi: 10.3109/17453678108992150.
van Moppes, F. I., & van den Hoogenband, C. R. (1982). Diagnostic and therapeutic aspects of inversion
trauma of the ankle joint. [Doctoral Thesis, Maastricht University]. Rijksuniversiteit Limburg.
Evans GA, Hardcastle P, Frenyo AD. Acute rupture of the lateral ligament of the ankle. To suture or not to suture? J Bone Joint Surg Br. 1984 Mar;66(2):209-12. doi: 10.1302/0301-620X.66B2.6368563.
Korkala O, Rusanen M, Jokipii P, Kytömaa J, Avikainen V. A prospective study of the treatment of severe tears of the lateral ligament of the ankle. Int Orthop. 1987;11(1):13-7. doi: 10.1007/BF00266052
Sommer HM, Arza D. Functional treatment of recent ruptures of the fibular ligament of the ankle. Int Orthop. 1989;13(2):157-60. doi: 10.1007/BF00266380.
Povacz P, Unger SF, Miller WK, Tockner R, Resch H. A randomized, prospective study of operative and non-operative treatment of injuries of the fibular collateral ligaments of the ankle. J Bone Joint Surg Am. 1998 Mar;80(3):345-51. doi: 10.2106/00004623-199803000-00006.
Pijnenburg AC, Bogaard K, Krips R, Marti RK, Bossuyt PM, van Dijk CN. Operative and functional treatment of rupture of the lateral ligament of the ankle. A randomised, prospective trial. J Bone Joint Surg Br. 2003 May;85(4):525-30. doi: 10.1302/0301-620x.85b4.13928.
Pihlajamäki H, Hietaniemi K, Paavola M, Visuri T, Mattila VM. Surgical versus functional treatment for acute ruptures of the lateral ligament complex of the ankle in young men: a randomized controlled trial. J Bone Joint Surg Am. 2010 Oct 20;92(14):2367-74. doi: 10.2106/JBJS.I.01176
Update Log
- March 2026: Page created on Ankle Evidence Hub
- Next scheduled update: June 2026 (or sooner ! if you know of a RCT in this field that meets our inclusion criteria – get in touch HERE)
