Ankle Sprain
Outcome: Recurrence
Comparison: Broström repair VS Broström repair with augmentation (suture tape or LARS)
Evidence snapshot
Volume
Data from 287 participants (4 RCTs)
Magnitude and Direction of effect
Very uncertain estimate
Statistical Fragility
Effect not statistically significant
Certainty of evidence
Risk of bias and serious imprecision
Support the project
If you found this evidence summary useful, you can support the continued development of independent evidence reviews.
Contributions help support ongoing literature surveillance, data synthesis, and site maintenance.
Evidence in detail
Inclusion criteria
- Randomized controlled trials
- Population: Adults with ankle instability (>3 months in duration)
- Intervention: Broström repair with augmentation (suture tape or LARS)
- Comparator: Broström repair
- Outcome: Re-injury (at least 6 month follow up)
Outcome definition and data extraction
Re-injury was defined according to the outcome measures used in each individual trial. Data were extracted at the longest reported follow-up. Analyses were conducted using the number randomised as the denominator, consistent with an intention-to-treat approach.
Effect measure and data pooling
Odds ratios (ORs) were calculated for each trial and pooled using a fixed-effects model. Statistical heterogeneity was assessed using the I² statistic, which quantifies the proportion of variability attributable to between-study differences rather than sampling error. Heterogeneity was negligible (H² = 0.63; I² = 0%), indicating consistent findings across the included trials. The test for homogeneity was not statistically significant (Q = 1.89, df = 3, p = 0.59), suggesting that the observed variability in effect estimates was compatible with chance.
Assessment of evidence quality and robustness
Risk of bias was evaluated using the PEDro scale. Certainty of evidence was evaluated using the GRADE framework.
The analytical framework underpinning this Living Review, including statistical methods and certainty assessment, is described in the Methods page.
Results
Included trials
4 RCTs involving 287 participants were included. (Trial characteristics in Appendix 1)
Follow-up ranged from 6 months to 5 years post surgery.
Effect estimate
The pooled estimate suggested a reduction in the odds of reinjury with augmented repair (OR 0.58), although the result was not statistically significant (95% CI 0.16 to 2.09; p = 0.41) and the confidence interval was wide, spanning potentially important effects in either direction.
Forest plot
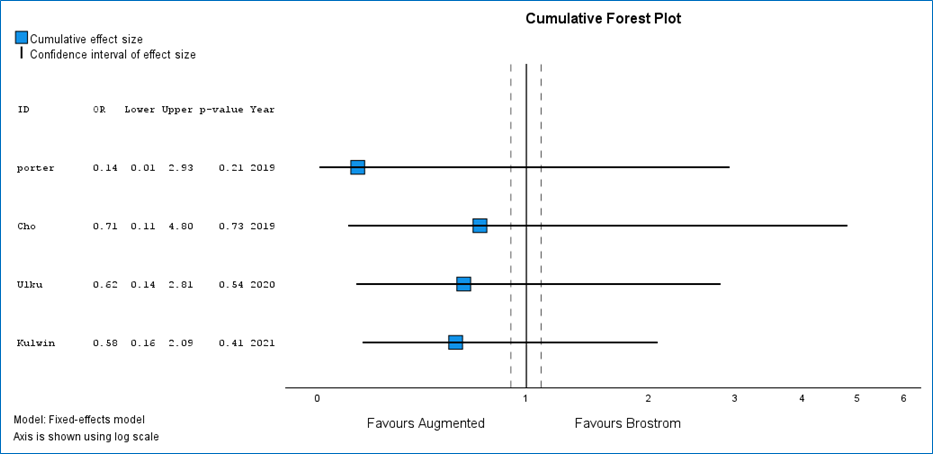
Heterogeneity
Statistical heterogeneity was negligible (I² = 0%; H² = 0.63), indicating consistent effect estimates across the included trials. The test for homogeneity was not statistically significant (Q = 1.89, df = 3, p = 0.59), suggesting that the observed variation between studies was compatible with sampling error rather than true differences in treatment effects.
Precision of pooled estimate
The precision of the pooled estimate was assessed by examining the width of the confidence interval around the effect estimate. The pooled odds ratio for reinjury was 0.58 (95% CI 0.16 to 2.09). The confidence interval was wide and compatible with clinically important effects in either direction, ranging from a substantial reduction to a possible increase in reinjury risk. These findings indicate considerable imprecision and substantial uncertainty regarding the true treatment effect
Fragility
A fragility analysis was not undertaken because the pooled effect was not statistically significant; fragility indices are typically calculated only for statistically significant results.
Publication bias
Publication bias was not assessed because the small number of included studies precluded meaningful evaluation using funnel plot–based methods.
Certainty of evidence
Certainty of evidence was rated as very low using the GRADE framework. Evidence was downgraded due to risk of bias, as reflected by PEDro scores below 7 in most trials (Appendix 1), and serious imprecision arising from wide confidence intervals and a small aggregate sample size. Further high-quality, RCTs are very likely to influence this estimate.
Interpretation
The pooled estimate suggested a reduction in the odds of reinjury with augmented repair (OR 0.58); however, the result was not statistically significant and the confidence interval was wide (95% CI 0.16 to 2.09), spanning potentially important effects in either direction. Statistical heterogeneity was negligible (I² = 0%), indicating consistent findings across the included trials. Despite this consistency, the estimate remains highly uncertain due to substantial imprecision and the small overall sample size. Taken together, the available evidence does not provide a clear indication that augmentation reduces reinjury risk following Broström repair.
Interpretation of these findings should consider the limited reporting of postoperative rehabilitation across included trials. Details regarding the content, intensity, and progression of rehabilitation were generally sparse or absent, despite rehabilitation being a key determinant of long-term functional outcomes following ankle ligament repair. Variation in rehabilitation protocols, or differences in the dose and progression of loading, may therefore represent an important unmeasured source of variability in the observed functional outcomes. As such, the contribution of surgical augmentation to functional recovery cannot be interpreted in isolation from the rehabilitation context.
Appendix 1: Characteristics of included studies

References (included studies)
Porter M, Shadbolt B, Stuart R. Primary ankle ligament augmentation versus modified Brostrom-Gould procedure: a 2-year randomized controlled trial. ANZ J Surg. 2015 Jan;85(1-2):44-8. doi: 10.1111/ans.12837
Porter M, Shadbolt B, Ye X, Stuart R. Ankle Lateral Ligament Augmentation Versus the Modified Broström-Gould Procedure: A 5-Year Randomized Controlled Trial. Am J Sports Med. 2019 Mar;47(3):659-666. doi: 10.1177/0363546518820529.
Ulku TK, Kocaoglu B, Tok O, Irgit K, Nalbantoglu U. Arthroscopic suture-tape internal bracing is safe as arthroscopic modified Broström repair in the treatment of chronic ankle instability. Knee Surg Sports Traumatol Arthrosc. 2020 Jan;28(1):227-232. doi: 10.1007/s00167-019-05552-w.
Kulwin R, Watson TS, Rigby R, Coetzee JC, Vora A. Traditional Modified Broström vs Suture Tape Ligament Augmentation. Foot Ankle Int. 2021 May;42(5):554-561. doi: 10.1177/1071100720976071.
Update Log
- March 2026: Page created on Ankle Evidence Hub
- Next scheduled update: June 2026 (or sooner ! if you know of a RCT in this field that meets our inclusion criteria – get in touch HERE)
